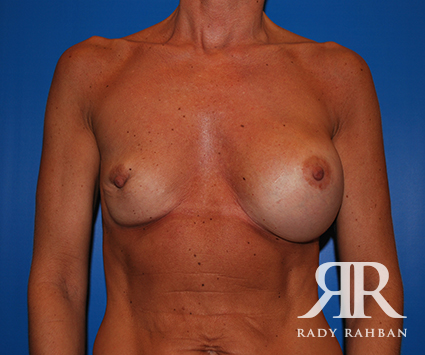
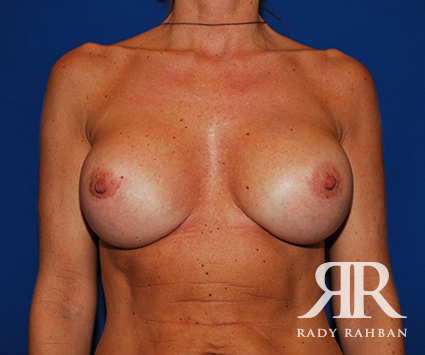
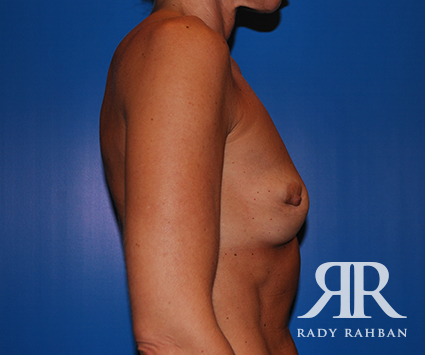
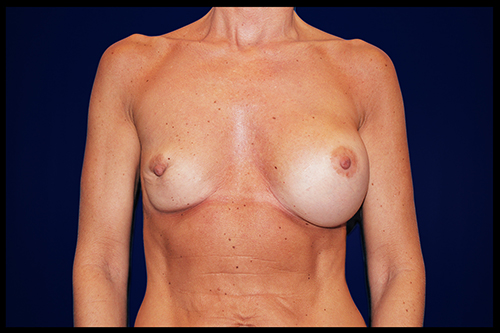
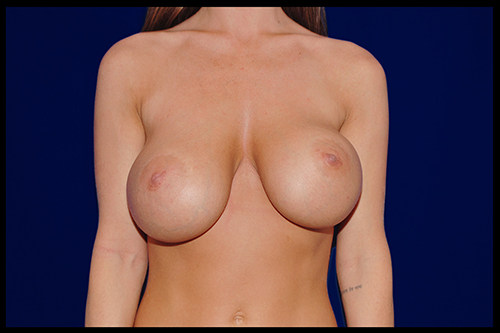
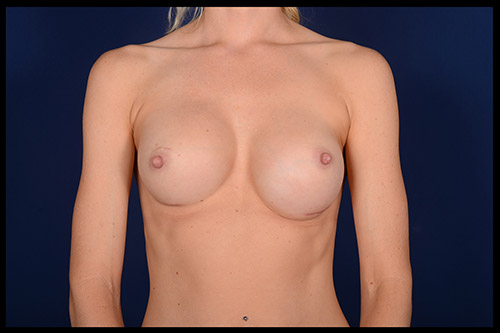
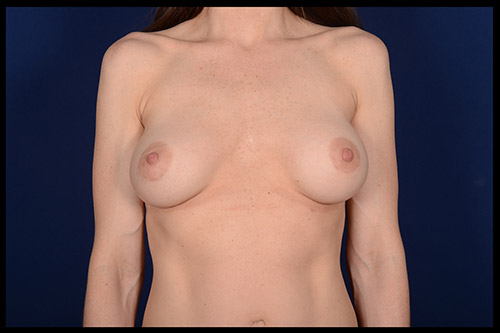
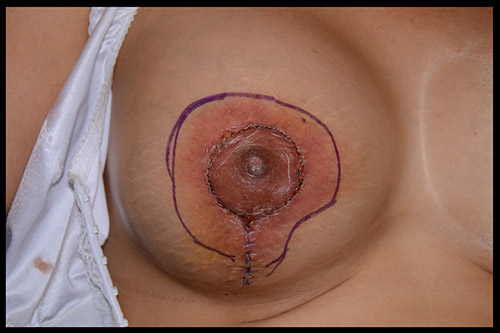
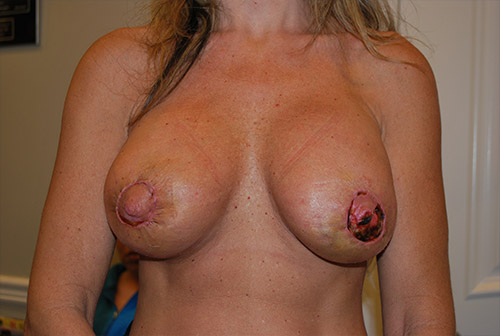
What is breast revision?
Also known as corrective breast surgery, breast revision is performed when previous cosmetic breast surgery does not lead to the desired results.
This may occur as a result of pregnancy-related changes that may have looked good prior to pregnancy but now no longer do. It may also be due to
recently done breast surgery that was done in error.
During breast revision surgery, the goal is to try to correct or reverse the elements that make the breasts unattractive. Unfortunately, not all
aspects are correctable and thus require the consultation of a skilled and knowledgeable plastic surgeon. Corrective surgery is considered one of
the most difficult areas of breast surgery, as you are not dealing with native tissue, but rather scarred or damaged tissue. However, Dr. Rady Rahban is not only a Los Angeles Mommy Makeover specialist, but his overall surgical specialty is in breast surgeries whether it is a breast augmentation after pregnancy, a Mommy Makeover breast lift or corrective surgery.
As expected, the complications associated with revisional breast surgery are much higher and sometimes the satisfaction rates are less--more so
than in any area of breast surgery. It is therefore important that patients do extensive research finding a surgeon who will tell them the truth and
not worsen their condition.
Patients with breast revisional issues are often vulnerable to unscrupulous or poorly skilled surgeons. This generally occurs because they are
overly eager to regain normalcy in their appearance, and they are less discerning. Patients are encouraged to remain meticulous in their choice for
a revision surgeon, despite the temptation to jump right into surgery. Since Dr. Rahban takes the care to encourage his patients to research far and wide, when patients do select him, they walk away with some of the best Mommy Makeovers Beverly Hills has to offer.
Am I a candidate?
In most cases, any woman who is unhappy with the results from a previous breast surgery is a candidate for breast revision. However, this can be broken down further. In many cases of breast revision, a complication arose following breast augmentation. However, sometimes a perfectly performed surgery can be ruined as a result of pregnancy and breastfeeding. Candidates like this may want to consider looking at Los Angeles Mommy Makeover procedures as an option. Such complications include:
Deflation or rupture
If a breast implant ruptures, it can create an asymmetrical, deflated appearance in the breasts, prompting the need for corrective surgery. This is much easier to detect with saline implants, as a deflated saline implant will likely go empty within 24 to 48 hours, creating an obvious asymmetry. With silicone, this may be more difficult to detect, and sometimes subtle in the change noted. One may need imaging studies like an MRI to be certain that a silicone implant has indeed ruptured.
Capsular contracture
This is the most common issue following pregnancy, as breast feeding and/or simple breast engorgement with milk can lead to this deformity. A capsular contracture is when the scar tissue around the breast implant becomes significantly hard, hence changing the shape and feel of the breast. Commonly, patients present with one or two breasts that have risen to the upper half of the breast and have become fixed and rigid on the chest wall.
Rippling
Rippling comes in two forms: palpable and visible. Most women have some degree of palpable rippling. That means when you feel your breasts, you can feel the implant to some degree. This is more common with saline implants than silicone implants. This usually occurs in the bottom of the breast near the inframammary fold, where there is no muscle present. Visible rippling occurs much more seldom and usually occurs in very thin patients who have very little breast tissue covering
Gross asymmetry as a result of any cause
This may be caused by capsular contracture, natural descent of breasts in different ways, or a host of other reasons.
Unsightly scars
Patients may have wide, thick or dark scars as a result of previous, poorly performed breast lifts, hence requiring excision and revision.
Bottoming out or “double bubble”
This deformity appears as a secondary bubble below the breast crease and is caused when the implant drops lower than it should. This can be the result of previous augmentation in a breast that likely needed a lift originally but was not done. In some cases, it can be caused by a breast lift or reduction that has settled with time, or caused by generally poor tissue structure and weak collagen support.
Lateral displacement, or side boob
This occurs when the breast pocket for an implant is oversized, hence creating two large a space for the implant to sit. Patients often complain that when they are laying down, their breasts fall into their armpits.
Symmastia or “uniboob”
This occurs when the skin over the sternum disconnects from the underlying layers, causing it to pull away from the sternum. This creates the appearance that the breasts are fused together in the middle. This occurs from an error in technique when the surgeon places the implants too close together, trying to create cleavage.
Oversized implants
Patients sometimes, either by their own choice or by an error of a physician, may be subject to implants that are much larger than they desire, and therefore may seek a smaller implant.
Extracellular matrix (ECM) is tissue from other sources, removed of all its cellular components, leaving behind a matrix or scaffolding of tissue. This serves as additional tissue when tissue is insufficient, such as when breasts have lost support or volume. It is used to create support like a mesh or a dam throughout the body, especially when trying to control a breast implant in a pocket.
When ECM is introduced, the body incorporates or sends cells into the scaffolding and makes it its own over the course of six to twelve weeks. At that time, it becomes biological and alive, whereas it begins as acellular, meaning not alive. It has become a crucial component of revisional breast surgery as well as breast reconstruction. More and more applications are being found for its use annually in the world of breast surgery. Your surgeon needs to be familiar with not only the various ECM products, but also how to use the material effectively. Unfortunately, this material is still quite expensive, and therefore should only be used when truly necessary.
Breast revision consultation
Note: while each surgeon approaches the consultation process differently, Dr. Rahban feels they should all have the same basic elements, ensuring patients leave very well informed regarding surgery. Below is how Dr. Rahban conducts a consultation.

Your consultation should be done by your plastic surgeon and not by his staff, such as his coordinator. In many cases, patients are offered free consultations, but you must understand that often means you’ll get a hurried consult. As a point of reference, Dr. Rahban on average spends up to an hour with each patient, reviewing not only what the patient came in for, but also explaining all the nuances such as the risks and alternatives to what that patient has requested.
There is no way to accelerate the dissemination of knowledge when it is so complicated and crucial.
During a post-pregnancy breast revision consultation, Dr. Rahban covers several crucial points. Firstly, he gathers data regarding what you consider to be the issue. He wants to ensure the correct result is gotten the second time around so no further revision is necessary. Second, after an examination, Dr. Rahban defines the exact problem, allowing you to better understand how you can benefit from a breast revision.
With a vast amount of experience with breast surgery, Dr. Rahban has seen all types of breast complications. The key with breast revision is correct diagnosis. Your surgeon must know what the problem is in order to give patients the correct options. As the breast tissue is no longer 100% normal, it is unforgiving and therefore an error in diagnosis will lead to a very poor outcome and make further revision even more difficult. Repeated revisional surgeries have exponentially worse outcomes, and therefore a patient should ideally seek revision only once.
As an extension of this, Dr. Rahban also reviews what patients should not expect from surgery. He is well known for telling his patients the truth and establishing a healthy level of expectation. Most patient dissatisfaction is related to inaccurate understanding and expectation of their surgery. Dr. Rahban deals in full disclosure to prevent this from occurring.
During a consultation, Dr. Rahban has one primary purpose—total patient education. He wants each patient to fully understand every nuance of breast revision surgery, as well as every risk and exactly how the procedure applies to them, allowing them to make the best decision for themselves. With his honest, candid approach, Dr. Rahban brings a new level of care to ensuring his patients know exactly how a breast revision works.
Breast revision procedure
Note: while no two surgeons perform this procedure identically, most techniques have a similar series of steps. Below is a brief overview of Dr. Rahban’s technique, allowing you to gain a more detailed understanding regarding how your surgery will be performed. The more you know, the more control you have.
Because breast revision after breastfeeding corrects any number of issues, there is no single procedure involved. It may be a combination of sophisticated procedures that need to be orchestrated in order to give you the desired result. Revisional surgery requires more knowledge, creativity and skill, as it is not routine surgery. Surgeries may involve exchange of implants, removal of capsular contracture scar tissue, repeat lifts, or correction of breast implant pockets. The following are some of the more common procedures to revise breasts:
-
The correction of capsular contracture requires either a capsulectomy or capsulorrhaphy. Dr. Rahban’s preferred approach is a complete capsulectomy. This involves removal of the entirety of the scar tissue, hence creating a brand new pocket without any of the old scar tissue.
Often, physicians will either do a partial capsulectomy or a capsulorrhaphy, which consists simply of making incisions in the scar tissue to release it. However, Dr. Rahban does not feel this is adequate and may lead to a suboptimal outcome.
A capsule may be very thick and sometimes even calcified. When performing a capsulectomy, it is critical that your surgeon take his time, as the capsule is very intimately attached to the surrounding tissue, such as the muscle and breast tissue. If this procedure is not done with care, damage can be done to the muscle and breast tissue, hence leading to contour irregularities and/or poor shape.
-
When an individual identifies a deflation, it should be corrected as soon as possible. This can often be as simple as removing the implant and replacing it. However, sometimes the capsule surrounding the implant needs to be removed as well. Additionally, if the implant is silicone and ruptures, the procedure becomes more complex as the silicone is difficult to remove. While the silicone is not dangerous to the human body, it is messy—all the reason why we recommend changing your implants every ten to fifteen years.
-
Symmastia is a very difficult problem to correct, so emphasis should be placed on prevention. There are two ways to correct symmastia. The traditional approach is to sew that area over the chest or sternum back down in an effort to close off the space between the implants. With this method, the implant will often break through the correction, hence creating a recurrence. Additionally, the shape of the pocket may be irregular, as it is very difficult to create a perfectly round shape.
The other, more advanced technique, is called a neo pocket formation. This is a very sophisticated technique whereby your surgeon will create a new pocket for your breast implant above the old pocket. This will allow him to close off the space between the breasts without the need for sutures. In both instances, your surgeon may choose to use ECM as reinforcement or support.
-
Correction of any asymmetry often requires a multiple technique approach. Sometimes the asymmetry is due to size issues and hence implants need to be changed. Other times it’s due to poor shape and hence different types of lifts need to be performed. As with all revisional surgery, many patients have issues with capsular contracture, and a capsulectomy is usually a part of the procedure.
-
Unfortunately, unsightly scars are a very common problem following breast surgery. All too often, patients are told that the cause for their unsightly scars is their poor healing, when in reality it was due to poor closure. In this instance, your surgeon would need to excise all of your scars and re-suture them using the multi-layered technique that’s described in the section on wounds and healing.
-
Correction of large implants may involve not only exchanging to a smaller implant, but may necessitate some type of lift procedure. When an implant is downsized significantly, the breast is left with excess tissue that, if not addressed with some type of lift, would lead to sagging.
-
The common complication of bottoming out or “double bubble” may be due to a variety of causes. Ultimately, some type of resuspension or lifting procedure will need to be done. This is usually in the form of a breast lift. If one of the causes is an oversized implant, then it is crucial that the implant be made smaller, otherwise bottoming out is almost certain to recur. If the patient’s breast tissue is very weak and thin, addition of extracellular matrix may be necessary for support.
-
Visible rippling is due to a lack of tissue at the implant-skin interface. This is common in patients who are quite thin or have very little breast tissue. While some type of lifting may tighten the breasts and reduce the visibility of rippling, often extra tissue in the form of extracellular matrix may need to be added as a buffer between the implant and the skin.
-
Lateral displacement of the implant has to do with over-dissection of the breast implant pocket at the time of formation. Similar to the symmastia, there are two methods of correction.
The first is suturing or closing the pocket with stitches in order to make the space smaller to accommodate the implant. The problem with this technique is that sometimes the stitches do not hold, and lateral displacement can recur. Additionally, there is the fact that it is difficult to create a smooth and round shape in the pocket using stitches.
Alternatively, there is a new and advanced technique called a neo pocket procedure, whereby your surgeon will create a new implant pocket above the old capsule that is smaller to accommodate the actual size of the implant.
Preparing for breast revision
For patients receiving a breast revision after pregnancy, preparation begins about a month before the procedure. Our office will provide you with a full list of actions to take as well as what to avoid. Each item on the list is intended to ensure you get a beautiful cosmetic result and that the surgery is as safe as possible. A few basic preparatory steps are listed below to give you an idea of what will be expected.
- Stop taking certain medications, such as aspirin and anti-inflammatories, as these can contribute to excessive bleeding
- If you are 40 or over, a mammogram is necessary in order to make certain that your breasts are in good health and that no underlying disease is
missed. If you have a family history of breast cancer, a mammogram at an earlier age may be indicated.
- Quit smoking, as this can slow the healing process.
- Make arrangements for the recovery process, including details such as a ride home following surgery
- It must be at least three months since the last time you’ve seen milk come out of your breasts.
- Breast augmentation patients should be relatively close to their ideal body weight.
If you have any questions prior to your surgery, our office is available to you. Call or email us any time, and we will help with anything you need. Our goal is for you to have a successful surgery, which we believe is contingent on research and preparation. Your success is predicated on doing your homework and being prepared. We strive to provide total peace of mind for our patients, as well as a safe, successful procedure.
Healing and recovery
Note: the recovery listed below is according to Dr. Rahban’s routine. Other surgeons may have a different approach to the recovery process.
Directly after surgery, you will awaken from anesthesia, at which point you will have little to no pain, as both the general anesthesia and the local anesthesia are still present in the breasts. You will have a surgical bra, as well as bandages underneath your bra. Dr. Rahban’s approach is to leave everything in place for one week until he sees you for your first post-operative visit.
During this initial period, many patients feel as though their incisions are getting dirty, causing them to wash the incision themselves. This is contrary to what should be done. When patients leave the operating room, the dressings are well secured and keep the incision sterile. Because most infections occur from contamination, patients who “clean” their wounds actually introduce bacteria from their hands and water, increasing the risk of early infection. Therefore, the incision will remain clean if the dressing is simply left alone, allowing the wounds to close on their own.
Learn more
Note: While some doctors may use drains, Dr. Rahban does not with his breast procedures. He feels that with meticulous hemostasis or control of bleeding and accurate technique, drains are not necessary with breast surgery. Only in rare cases of complex revision does he use drains.
At one week, you will see Dr. Rahban, at which time your bandages will be removed along with most of your sutures. He will then begin telling you how to care for your incisions. Refer to Dr. Rahban’s scar management protocol for more information.
During the initial post-operative one-week period, you’ll have bandages on. The surgical bra will be tight and there will be moderate pain. If you received implants, there will be fullness at the top of your breasts. Over the next 6 weeks, the fullness will settle, but the breasts will not fully settle for about three months. If your breast revision required a dual plane approach, the breasts eventually settle into a teardrop shape.
Most patients return to work after about 7 days. During this time, you will still be wearing your surgical bra, but it can be taken off to shower. It may seem counterintuitive, but there is nothing magical about this bra. It does not hold the breasts in a specific position, nor does it provide proper support. In fact, it’s what this bra DOESN’T do that makes it special. If a normal bra or sports bra were to be worn during this period, it may lead to the breasts healing in a higher position than one would like. Therefore, this surgical bra ensures the breasts heal properly and that you get the best cosmetic result from breast augmentation.
The second visit occurs at 2 weeks after your surgery, at which time your pain is significantly less, and the focus is on wound care. During this visit, Dr. Rahban will continue to ensure you know how to care for your incisions. As many of his patients come from out of town, it is usually this two week milestone that marks their return home. Ideally, he wants patients to remain close to his office for the first two weeks after surgery to monitor their healing and ensure they are on the right track.
At 6 weeks you should essentially have no more pain. Your scars should be well healed, and therefore you can begin to resume all previous activities with the exception of lying completely flat on your breasts, such as during a massage. Dr. Rahban doesn’t recommend this kind of activity until 3-5 months after the procedure.
By this 6-week mark, implants have begun to settle and have a more natural appearance. However, they may still not have the final teardrop appearance that you are looking for. You will be able to resume all strenuous activities and exercise. Additionally, you will be able to buy your first set of bras, as you will be wearing the surgical bra until this point.
Note that at this juncture, your scars will start to become more inflamed, and perhaps more obvious, as your body is beginning to do its healing work. Refer to Dr. Rahban’s timeline on wound healing in the wounds section for more information.
At 3 months the implants and tissues will have fully settled and you will have obtained your desired shape. That being said, your scars will most likely be slightly redder or more colored and inflamed. This is because your body is now at its peak of healing. Therefore, it is important for patients to understand the healing process and that it takes time for scars to fade. In fact, this process can take over a year. Please refer to Dr. Rahban’s timeline on wound healing for more information.
After one year, Dr. Rahban schedules the final follow-up appointment. Dr. Rahban believes strongly in this appointment, because it allows him to do a final breast check and make sure that everything is how it ought to be. This also gives Dr. Rahban an opportunity to check on the scars, allowing him to know his final result.
Most doctors should be able to see their patients at the end of a year so they can assess their work. If a physician is not seeing you once you are completely healed, he can’t see his final results and therefore refine his technique. It takes a year for the wounds to heal, and your surgeon should be seeing you at that time.
At this point, Dr. Rahban checks the integrity of your breast implants and makes sure everything is as it should be. He makes sure there is no scar formation or any other complication such as rupture.
If your breast revision required implants, it’s recommend they be replaced every 10 or 15 years. While there is no exact time, it’s good to remove them before they break. If they do break, it is not dangerous, but they are a little more complex to replace.
For his out of town patients, Dr Rahban is flexible and will schedule follow ups around their ability to visit him. He knows that travel and time off of work requires coordinating, so his staff will make sure to assist with follow ups. If need be he can even utilize telemedicine technology such as Skype or Facetime.
Your relationship with Dr. Rahban continues long after your breast revision is over. At any point after your surgery, he and his office are available to help with any questions or concerns that arise. Even several years later, his door is open to patients who have concerns about their implants.
Breast revision risks
Because all breast revisions are different, each of the following risks may not apply. Breast revision risks include but are not limited to:
Infection
Also quite rare, infection is thoroughly combatted before, during and after surgery. The night before surgery, we have patients wash themselves with an antiseptic soap. We give patients antibiotics directly prior to surgery, as well as after surgery. Additionally, Dr. Rahban has very strict post-operative instructions regarding wound management that he believes reduce the risk of infection.
Asymmetry
This means the right and left breasts will not be identical in size or shape. No two breasts are ever identical before surgery, nor will they be after surgery. The goal, however, is for the breasts to be very close in size and shape. Hence, if there is any asymmetry to begin with, Dr. Rahban will attempt to correct it. This may include using different sized implants, and/or the removal of more tissue from one breast.
Rippling
Rippling comes in two forms: palpable and visible. Most women have some degree of palpable rippling. That means when you feel your breasts, you can feel the implant to some degree. This is more common with saline implants than silicone implants. This usually occurs in the bottom of the breast near the inframammary fold, where there is no muscle present. Visible rippling occurs much more seldom and usually occurs in very thin patients who have very little breast tissue covering their implants. Visual rippling usually occurs on the outer part of the breasts near the axilla.
Rupture
Over time, breast implants can rupture. However, the rupture rate with the new generation of implants is quite infrequent and rare. Despite this, it is recommend that patients replace their implants every 10 to 15 years.
Nipple-areolar complex necrosis/death, also known as gangrene
While this is the most dreaded complication, it is extremely rare. In order to manipulate the nipple areola complex during a breast revision, the nipple-areolar complex must be released from some of its surrounding tissue. Therefore, great care must be taken in order not to be overly aggressive. Other factors which may increase the risk of this complication include:
Scars
While an inevitability of surgery, the issue is not whether you will have a scar, but rather the quality of your scar. The goal is for you to have a well-healed, faint or fair scar with time. In order to prevent the unsightly scar that so many people are worried about, Dr. Rahban takes steps to minimize it.
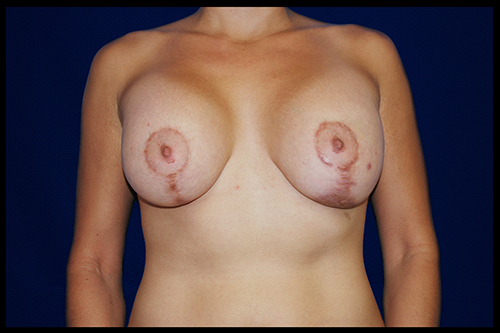
Dr. Rahban believes in a 50-50 rule. Fifty percent of scar healing has to do with the technique of your surgeon’s closure, or how well the incised tissues are brought back together. The other fifty percent is the patient’s biology. Because a patient has little control over her biology, there is a lot of emphasis placed on your surgeon and his closure technique. While many surgeons place their emphasis on post-operative scar management, there is very little science that any of these modalities actually work. Therefore, Dr. Rahban focuses on an unusually fastidious closure technique to ensure that all tissues heal with minimal scarring.
Please refer to his timeline on wound management for more information.
Capsular contracture
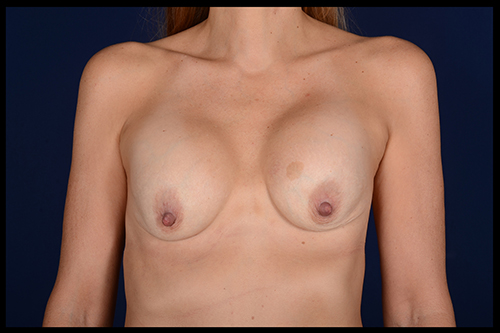
The rate of capsular contracture when the implant is placed below the muscle is approximately 5% to 15% and approximately 40% when placed above the muscle.
When an implant is placed within the body, the body recognizes it as a foreign object. Therefore, it tries to protect you from the foreign material. It does this by creating a capsule or scar tissue around the implant. Any medical device that goes into your body, such as a pacemaker, a prosthetic knee, or a heart valve, causes the body to create a capsule or scar tissue around it. Therefore, all women with breast implants have this capsule.
While certain capsules don’t create a cosmetic issue, some women create a thicker capsule than others. This is not a rejection, but rather the body making a more aggressive scar tissue envelope. This can become of concern to the patient when the capsule causes the implant to feel firm and sometimes displace or move the implant upwards, creating an unsightly breast. The degree of capsular contracture can vary from mild to severe. When it is severe, the only solution is to remove the scar tissue and replace the implant. While this phenomenon can recur, one often doesn’t reproduce the capsular contracture.
Massaging the breasts has never been proven to reduce the rate of capsular contracture. While many patients think that massaging the breast will reduce the risk of capsular contracture formation, unfortunately there is no science that shows is the case.
Bleeding
This is a very rare complication. Despite this, we take action to minimize the risk as much as possible. This primarily includes having the patient stop all medications that promote bleeding at least two weeks in advance, such as anti-inflammatories, aspirin and supplements.
Loss of sensation to the nipple
The loss of sensation to the nipple has nothing to do with the incision used in the breast revision. The majority of the sensation to the nipple comes from the fourth intercostal nerve located near the armpit within the breast pocket. Most loss of sensation is due to picking too large an implant and therefore damaging the nerve when the pocket for the implant is created. Of course this is primarily applicable when one gets a breast implant during her post partum breast revision.
Decreased breast milk
With most types of breast revision, some amount of breast tissue is incised, thereby cutting breast milk ducts. Therefore, some degree of breast milk reduction can be anticipated. Unfortunately the degree of reduction is difficult to predict prior to surgery. Many patients are still able to breastfeed after a breast revision.
- Smoking
- General poor health such as diabetes and heart conditions
- Adding an implant. This can increase the risk of this complication because it creates tension under the NAC, thereby reducing some of its blood
flow. This is why Dr Rahban is opposed to overly large implants with lifts. He spends a lot of time with patients going over sizing for this
reason.
In the case of a capsulectomy
it may lead to contour irregularities and divots if not done correctly. Additionally, if a capsulectomy is done too aggressively, it can create a breast pocket that is too large, causing a new host of problems.
Breast revision cost
There is no standard cost for a breast revision as there are many unique variables. Below is a list of the elements that will determine the cost of your procedure so you understand what exactly you are paying for.
- The skillset of your surgeon. Is he or she a plastic surgeon or a cosmetic surgeon? Is he or she board certified? A board certified plastic surgeon will often be more expensive.
- How long it takes to perform the procedure. Generally the faster your surgeon, the less facility and anesthesia fees and the greater the surgeon’s profit. Therefore, surgeons have an incentive to work more quickly. When it comes to surgery, faster is not better. Be sure to ask your surgeon how long the procedure will take and be wary if it seems too quick. The average time for breast revision is: 3-6hrs.
- The anesthesia provider. There are many types of anesthesia providers. An anesthesiologist who is a medical doctor will be more expensive than a nurse anesthetist. Do your research and find out who provides anesthesia for your plastic surgeon. Dr Rahban is partial to using an anesthesiologist as opposed to a nurse anesthetist.
- The facility in which your operation is performed. Unfortunately, surgery centers and hospitals are not all created equal. The more sophisticated the facility, the more expensive its hourly fee. Facilities that are Medicare-certified tend to be more costly as well.

Questions to ask your surgeon
Below are specific questions to ask your surgeon during your consultation. Each of these will allow you to understand his or her approach and thus make an informed decision. To print these questions so you can ask your surgeon, see link below to download a copy take with you to your consultation.
What is my exact diagnosis? How will you fix it?
With a vast amount of experience with breast surgery, Dr. Rahban has seen all types of breast complications. The key with breast revision is correct diagnosis. Your surgeon must know what the problem is in order to give patients the correct options. As the breast tissue is no longer 100% normal, it is unforgiving and therefore an error in diagnosis will lead to a very poor outcome and make further revision even more difficult.
Will my breast revision require the use of extracellular matrix?
Extracellular matrix (ECM) is tissue from other sources, removed of all its cellular components, leaving behind a matrix or scaffolding of tissue. Your surgeon needs to be familiar with not only the various ECM products, but also how to use the material effectively. Unfortunately, this material is still quite expensive, and therefore should only be used when truly necessary.
If I’m reducing my implant size, will you also lift my breasts?
Correction of large implants may involve not only exchanging to a smaller implant, but may necessitate some type of lift procedure. When an implant is downsized significantly, the breast is left with excess tissue that, if not addressed with some type of lift, would lead to sagging.
Do you offer a second consultation prior to my procedure?
Every patient goes through a thorough pre-operative process. This begins with a pre-op visit two weeks prior to surgery. This is similar to a second consult. During this time, you will go over the details of your surgery with Dr. Rahban, and you will get a second opportunity to ask questions and go over your procedure, thus ensuring a complete understanding.
How many follow-up appointments do we have?
After a breast revision after childbirth, Dr. Rahban schedules a total of five follow-up appointments. Most plastic surgeons schedule two follow-ups, during which time you may not even see the doctor. During every follow-up appointment, Dr. Rabhan sees his patients personally.
Download questions